WA women are leaving it longer than ever before to become mothers. But should they be waiting till they’re ready? And is a last-ditch bid to ‘have it all’ worth the price?
I blink awake from the fog of general anaesthesia. My lower abdomen, swollen from egg-collection surgery, throbs under crimson contusions. A fertility specialist approaches with a sympathetic smile. "Just three eggs this time, love. Better than none."
Two interminable weeks later, I learn that the sole embryo resulting from this round of IVF hasn't taken. I'm thousands of dollars poorer. And I'm still not pregnant.
Until an embarrassingly late age, my life's only ambition was to become a mother. My own mum had her first child at 21, and my grandmother had hers at 20. I liked the sound of that – until I grew up, of course, and things like university, travel, more university and a career caught my eye. It wasn't until my husband and I both hit 30 that we took a breath and realised we were desperate to become parents. Immediately.
At first it was fun. I had spent my twenties sure that I was one broken condom away from getting knocked up, so unprotected sex was a thrill. Not falling pregnant in the first three months shocked me. A miscarriage six months later broke my heart.
I suffered through baby showers and first birthday parties. The continuous stream of babies' faces on my Facebook feed mocked me. Meanwhile, my husband endured my monthly breakdowns, the new role of sex in our lives (dictated by ovulation apps, thermometers and soothsaying naturopaths), and his own devastation at not yet being a father.

Embryologists at work in the lab at PIVET Medical Centre in West Leederville.
The most demoralising moment came three years later, when specialists threw up their hands and labelled it 'unexplained infertility'. It didn't make sense. I was 33 and healthy. Everything I had achieved thus far had come from hard work and determination, and yet I couldn't manage the one thing I assumed wouldn't take any effort at all.
So we turned to in vitro fertilisation (IVF), an expensive and invasive process that transformed me into a nervous, hormonal wreck, my thighs covered in bruises from the daily hormone injections, the veins in my arms speckled with scabs thanks to the constant blood tests. I became a human pincushion, a lab rat, a shell of a woman.
How did I get here? Had I not paid attention the day the sex ed teacher gave the lesson on fertility? Had my gynaecologist forgotten to warn me that time was ticking away? Or had I simply been too busy to give a thought to family planning?
Whatever's to blame, one thing's for certain: I'm not alone. According to the Australian Bureau of Statistics, in the last three decades, the median age of Australian women giving birth has increased from 25.4 to 30.7 years. These women are choosing, like me, to spend their youth partying, travelling, studying, climbing the corporate ladder, buying property and eventually – once all their ducks are lined up – finding their soulmate and starting a family.

Dr John Yovich, founder and medical director of PIVET Medical Centre.
It's not a purely selfish decision. Waiting until you're financially and emotionally prepared to bring life into an already overpopulated world isn't foolish. It's responsible. The problem comes from assuming that parenthood is schedulable.
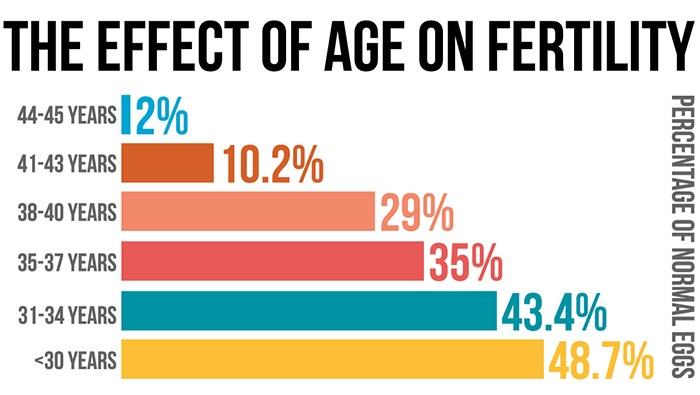
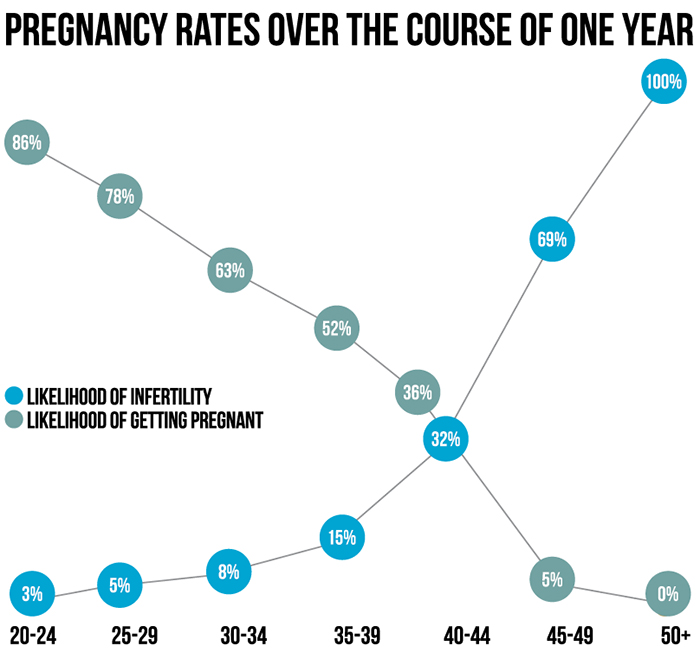
The brutal truth is that while women possess about 300,000 eggs at the time of their first menstrual cycle, 88 per cent disappear by age 30, and 97 per cent by age 40, according to a study by the University of St Andrews and Edinburgh University. A woman in her mid-twenties, the age when fertility peaks, has a 20-25 per cent chance of conceiving per cycle. That drops to below 10 per cent at age 35, and just 5 per cent at age 40.
"Society is suffering because of women's need to 'have it all', but you can't have it all," says retired Perth obstetrician Margaret Smith. I'm sitting in the formidable octogenarian's West Leederville living room, which is crowded with framed photo collages of the countless babies she's delivered over her half-century career.
"In my day, women didn't go for careers – you'd get married and have children. I did medicine, and I had to make a decision for myself – am I going to stop and have kids or not? And the answer was no.

Retired obstetrician Margaret Smith believes society is suffering from women's need to 'have it all'.
"But girls nowadays don't want to make that tough choice, they think they can go on having everything – 'I'll go on the Pill, I'll keep changing partners, I'll build my career' – but no one's actually told them the facts.
If you wait until you're 40, even if you do IVF, your chances are not very good. The egg numbers have gone. Sorry!"
Margaret places some of the blame on the Pill. "Sure, it was a major breakthrough in the sixties. Everyone thought, 'Hooray hooray, we can stop unwanted pregnancies', but it stopped a lot of girls from even thinking about pregnancy until it was too late. The Pill has a lot to answer for."

Grae and Peter Hastings (seen here with their baby Atreju) intend to donate their unwanted embryos to those who cannot conceive their own.
Cailin Jordan, Perth psychologist and fertility counsellor, often encounters this with her clients. "We've been brought up on a lot of myths: how you can have it all, and how important career is," says Cailin. "But you can pause parts of your career and pick it up again – you can't pause your fertility. You can't turn the clock back. I frequently work with women in their 40s who are full of regret, saying, 'I was waiting for XYZ scenario that was going to make things ideal for doing this.' Sometimes, when you dissect it with people, you find that there's actually never a 'right time', but a fantasy of how life has to look."
Headlines proclaiming older celebrities' miraculous pregnancies don't help. Personal trainer Michelle Bridges is due to become a first-time mother at 44; television presenter Sonia Kruger had her first bub at 49 (with the gift of donor eggs from a friend); and photographer Annie Leibovitz gave birth to her first child at the ripe age of 52 using a sperm donor, then twins at 56 by a surrogate.
Dr Simon Turner, a Perth obstetrician and gynaecologist, and the medical director at Hollywood Fertility Centre, deals with the fallout almost daily. "Those one or two celebrities are held up as examples of what any woman can do," says Simon. "They perpetuate the lie that you can easily get pregnant later in life."
Other couples wrongly believe that advances in modern assisted reproductive technologies, like IVF, hormone treatments and artificial insemination, offer an infallible 'safety net'. The booming industry is currently worth $4.8 billion worldwide, and is projected to reach $36.9 billion by 2019. According to reports from market research firm IBISWorld, women over 35 (the age when fertility starts to plummet) make up 58 per cent of that market.

Perth GP Belinda, seen here with her boys Thomas and Cooper, endured 14 rounds of IVF before conceiving.
In WA, each round of IVF costs between $8000 and $10,000 – roughly half of which is covered by Medicare. Considering it takes an average of three IVF rounds for a woman to fall pregnant, it's no small damage to the pockets of couples and taxpayers alike.
But the industry's skyrocketing growth is more indicative of global demand than effectiveness. In fact, The European Society of Human Reproduction and Embryology reports that, on average, only 350,000 of the 1.5 million assisted reproductive cycles worldwide result in a live birth. That's a global failure rate of 77 per cent. In Australia, it's a grimmer 82 per cent, according to a 2014 University of NSW report.
That dismal truth is something Perth lawyer Jessica*, 34, knows all too well. Parents to beautiful one-year-old Sean*, she and her husband Paul* were 30 and 34 respectively when they started treatment at Fertility Specialists of WA in Claremont. The doctors found Jessica had multiple fertility issues, including ovulation irregularity, low egg reserves and a uterine malformation.
"The first round of IVF was really eye-opening," says Jessica, staring into her coffee cup. We've met at a bustling suburban cafe in Shenton Park. "I really struggled with all the drugs. I got ovarian hyperstimulation syndrome, which caused horrible bloating and headaches, and my emotions were really, really heightened from all the hormones, not just during the process but afterwards. So they had to give me even more drugs to counteract it."

Of the 14 eggs harvested from the collection surgery that first round, none survived. "It was incredibly disappointing, and from that point onwards I don't think my body ever really recovered."
Fast-forward two and a half years, four egg collection surgeries, six failed embryo transfers and three miscarriages later.
"By that stage, I was just a mess. I was having night sweats and panic attacks, my hair was falling out. It was the stress, the drugs, the hormone manipulation, and the fact I'd been doing it so long. I mean, by the time I fell pregnant with Sean I had gone under nine general anesthetics. That's ridiculous."
Although not necessarily recommended by her fertility clinic, Jessica opted to act on a friend's suggestion and visit a Nedlands Chinese medicine practitioner who specialises in fertility issues.
"We went through my whole history together and I said I was about to go in for my seventh transfer. The practitioner basically just stopped the whole process for me, saying, 'What you're trying to do is run a marathon without doing any training. It's almost certainly not going to work, even if you have the best embryo. Your body is too exhausted.' It was the biggest wake-up call – he was so right."
He had Jessica drink special tea three times a day, quit alcohol, coffee and sugar, and take up gentle exercise instead of the intense running and spin classes she'd been doing. Six months later, Jessica went in for the transfer and – voilà – she fell pregnant with Sean.
"I felt so much better going into that last round. As well as being in a much better place physically and emotionally, we also decided to undertake an advanced embryo selection test called CGH (Comparative Genomic Hybridisation) Array. It was really expensive – over $5000 out of pocket – but at that point we were like, 'Whatever. What's another five grand?'" she says with a wry laugh.
The screening process required that a single cell from each of the eight fresh embryos collected be sent to a Melbourne lab, where every chromosome was tested for genetic abnormalities. The results, which came approximately 48 hours later, revealed which of the eight embryos were viable. Jessica's fertility doctors believed that most if not all of them would have been deemed viable and frozen for later transfers if they had not undergone the more rigorous form of testing, but the genetic screening showed that only two, in fact, were viable for transfer.
"It's crazy," says Jessica. "If we hadn't had them tested, we could have gone through another six failed embryo transfers. Personally, after the journey we went through, I'd never touch IVF again without it."
Even those fortunate enough to fall pregnant through assisted reproduction often report a significant downside: paranoia that they won't carry the baby to term; fear of trademark complications of 'older' pregnancies, such as chromosomal abnormalities; or anxiety about a perceived lack of control over the process.
Few health practitioners in Perth have dealt with as many older mums as Tim Jeffery, one of Perth's most trusted obstetricians, with more than 30 years of experience delivering babies out of St John of God in Subiaco. Operating a private practice, he says the majority of his patients are professionals in their mid-to-late 30s.
Intuition would tell you that older mothers make better mothers, because they've got more financial security and life wisdom, but Tim believes age works against them in more ways than one.
"Older first-time mums are much more aware of the risks of having a baby late, so they're more likely to be anxious," says Tim. "Especially if they've had a career where they've been in control and suddenly that's taken away from them. They find it very difficult to go from being in control to being controlled. Maybe they have feeding trouble, or the baby screams all night. Their expectations are much higher and, when they aren't met, postnatal depression is much more common.
"If I look after someone who's around 18-20 years old, which doesn't happen
very often, they sail through the pregnancy, they sail through the labour, they sail
through the delivery. They're much, much more adaptable."

But what about the women who are ready for motherhood at the ideal age, but haven't yet found a partner? A growing number are putting their fertility on ice – literally – using egg-freezing technology. The process was originally developed in the 80s as a way of helping to preserve the fertility of women undergoing damaging cancer treatments like chemotherapy. It comprises freezing a woman's eggs, and then, once the woman regains her health, thawing and fertilising an egg, and implanting the resulting embryo.
The technology has since been appropriated for the benefit of those
suffering from so-called 'social infertility': women with healthy eggs but less-than-ideal circumstances. This theoretical 'pause button' on fertility is being hyped as an empowering silver bullet – much like the Pill – giving women control of their private and professional lives.
In the US, egg freezing has gone mainstream, largely thanks to The American Society for Reproductive Medicine's decision in 2012 to no longer consider the process 'experimental'. Technology giants Apple and Facebook (along with Citibank and JP Morgan Chase) offer the procedure for female employees, encouraging women to "lean in, but freeze first." At the same time, egg-freezing 'parties' are on the rise. There are even reports of parents giving daughters the procedure as a birthday or graduation gift. But many question whether the treatment is luring women into a false sense of security. After all, there's no guarantee those eggs, once thawed, will result in a live birth.
Dr John Yovich, founder and medical director of PIVET Medical Centre, is optimistic. His clinic pioneered IVF in Perth (WA's first IVF baby, Jarrad Carter, was born in 1982), and was the first in Australia to introduce an egg-freezing technique known as vitrification. The method, which was originally developed in Japan, ensures a 90-95 per cent egg survival rate, compared with 50-60 per cent of more conventional, slow-freezing methods. Even more impressive, pregnancy rates using vitrification are comparable to that of fresh eggs.
However, John explains that success depends entirely on the age of the woman at the time she freezes them. "Egg freezing is a great option to maintain fertility, so long as the woman does it by the time she's 32 years old. If she provides us 20 eggs then there's about an 80 per cent chance that we can later generate a successful pregnancy.
"The majority of women who come to us at the moment have only just read about egg freezing, and come rushing in because they're knowledgeable, but aged
39 or 40. But by then their ovaries have passed their prime, with depleted egg numbers – the remaining eggs have lower quality, and their chances of pregnancy are low. They would need to freeze 40 eggs to have anywhere near that 80 per cent chance; and more eggs if they are over 40."
Age isn't the only factor. There's also the steep price, none of which Medicare covers. In WA, freezing your eggs will set you back around $10,000 – more, if multiple surgeries are required to produce the critical mass of eggs. Then there's the annual cost of around $300 per year to store them. That's one expensive insurance policy.
Vitrification is also being used around the world for the donation of sperm, eggs and embryos to couples unable to conceive on their own. Demand is extremely high for these donations, but Australian law dictates that donors' identities be disclosed. If couples don't have any family members or friends willing or able to donate, they're waitlisted for third-party donations, which are rare.
Lucky there are people like Grae and Peter Hastings. Unlike most couples who have their unwanted embryos destroyed, the Hastings are donating theirs to complete strangers, well aware that those future children might come knocking at their door one day.
The Mount Lawley couple knows firsthand how harrowing the infertility journey can be. Grae, now 34, and Peter, 33, spent three years trying for a baby naturally before doctors diagnosed them with male-factor infertility as a result of a hernia Peter suffered as a child.
Like Jessica, Grae suffered an extreme case of ovarian hyperstimulation syndrome during her first egg-collection surgery, causing her to be bedridden for three weeks and to endure a level of physical pain she insists was "way, way worse than childbirth". Nevertheless, the surgery resulted in 10 viable embryos, and Grae fell pregnant during that same round. The result? A beautiful 18-month-old boy by the name of Atreju.

"We're going to do one more round of IVF and have another child, and then we're donating the remaining embryos to other couples who can't conceive," says Grae.
"They're eight solid, healthy embryos. A lot of people would just destroy them,
but I'm not OK with that. I realise that, in a way, we're 'giving away' our biological children, but after going through the pain of wanting a child and not being able to have one, and the pain of IVF… I don't understand how people could deny other couples that opportunity."
Nevertheless, some couples find it impossible to let go of the dream of parenting their own biological children. Take 36-year-old mother of two and Perth GP, Belinda. She and her husband, Chris, underwent a harrowing 14 rounds of IVF, half at Fertility North, and half at Fertility Specialists of WA.
Being the eldest of nine children, Belinda always knew she wanted to be
a mum. "I planned my whole life around being a mother," she says. "I mean, I even chose a career that would fit around having kids. I truly didn't know who I'd even be without them.
"The psychologists would always ask me how long we were willing to go on, but
I couldn't even contemplate the idea of giving up. It was just too important to me. If I gave up, then it was like I was giving up on being a mum. And I couldn't do that."
Luckily she didn't. Her three-year-old son Thomas was born after 13 rounds, and 18 months later she gave birth to her second son, Cooper, which took only a single round of IVF. If there's one thing her painful journey instilled in her, it's a fierce appreciation for motherhood. "I still, to this day, feel so grateful," says Belinda. "I just love every minute of being a mum because for so long I didn't know if I'd get to be. It's so precious."
Unfortunately, some couples never succeed. Stepping in and calling time is one of the hardest tasks that a fertility specialist faces. Dr Simon Turner remembers one occasion very clearly.
"I had one patient that had fertility treatment for eight or nine years," says Simon. "I finally sat her down and said, 'That's it. I'm giving up. There's no point going on. Your eggs are gone, your hormone levels are in the menopausal range, you have no follicles left." Well, some years later, at 46 years old, she rang me saying, 'Dr Turner, I'm pregnant'. You could have picked me up off the floor. I thought she would tell me about some new herb she had found in the back garden, or some revelation. No. She told me she and her husband were on a trip, found two bottles of fine Champagne, screwed themselves stupid in a drunken fit, and that was that."
"That makes me feel like I know this much about infertility," Simon says, holding his fingers close together and letting out a roar of laughter. "There's someone in the heavens that's got their finger in the pie. Because why would a 46-year-old lady, seven years after I gave up, and after nine years of treatment, get pregnant in a dirty weekend? It makes no sense, but it's great, because it shows that you can never lose hope."
Dr Turner needn't be so modest – it was thanks to him and the team at Hollywood Fertility Centre that I fell pregnant on my second round of IVF. As I write this, we're just weeks away from meeting our firstborn. Something tells me our four-year ordeal will be nothing in comparison to the challenges of parenthood that lie ahead. You won't hear me complaining.
ALTERNATIVES TO IVF
Infertility – the inability to conceive after at least a year of trying – affects
one in six Australians. If assisted reproductive technology, such as IVF, fails to work, then what options remain?
DONATION
Sperm, egg and embryo donation is available to infertile couples in Australia, though it's not very common, due to the fact that all donors must agree to release their identity, which any child born of their donation can access once they reach
18 years of age. Many couples, therefore, ask family or friends to donate, or visit countries such as South Africa, Italy or Spain, which offer anonymous donation.
SURROGACY
Australia allows for 'altruistic surrogacy', in which the surrogate receives no financial gain for carrying a child. However, because Australian law recognises the birth mother as the mother of the child – regardless of genetics – a surrogate is legally allowed to change her mind and keep the baby if contracts aren't in place. For this reason, some couples opt for surrogates outside Australia, such as in India or Russia.
ADOPTION
Adoption in Australia is a notoriously difficult and lengthy process. It's also on the decline. According to a 2014 report by The Australian Institute of Health and Welfare, there's been 76 per cent drop in adoptions in Australia in the last 25 years. In fact, last year saw just 317 children adopted. This is largely blamed on the inherently long wait times due to heavy government regulations. Adopting a child from overseas, for example, takes an average of five years.